First Opioid Rx Leads to Long-term Use in 1 of 5 with Rheumatic or Musculoskeletal Disorders
Patients with rheumatoid arthritis and fibromyalgia were at the greatest risk of transitioning to long-term opioid use 1 year after a first prescription, a new study found.
Among primary care patients with rheumatic and musculoskeletal disorders (RMDs) prescribed an opioid for the first time, as many as 1 in 5 transitioned to long-term opioid use within 12 months of the initial prescription, report British investigators.
In the study of more than 800 000 people, those with rheumatoid arthritis and fibromyalgia were at the greatest risk of continuing on to persistent use after an initial opioid prescription, with up to 1 in 3 persons meeting the criteria after 1 year.
The findings are from a research letter published online May 16 in the Annals of Rheumatic Diseases.
“Health professionals should be aware of the high proportion of long-term opioid use in patients with RMDs. Introduction of prompt interventions, such as medication reviews or de-prescribing, to ensure the appropriateness of long-term opioid therapy, and proactive consideration of non-pharmacological treatments for pain relief would also be of benefit to reduce avoidable harms in this patient population,” wrote lead author Meghna Jani, MRCP, PhD, a National Institute for Health and Care Research fellow and clinical senior lecturer at the Centre for Epidemiology Versus Arthritis at the University of Manchester, and colleagues.
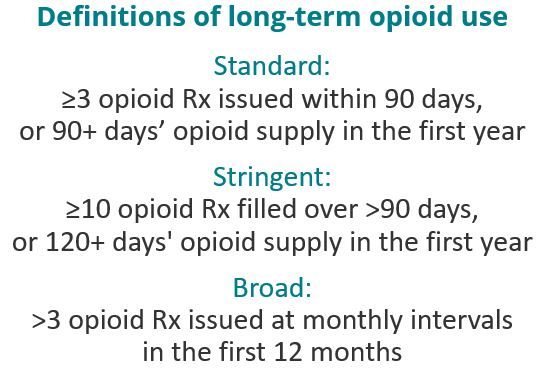
Jani et al point out that most research defines long-term opioid use as ≥90 days but that definitions in the literature vary widely, making it difficult to characterize the scale of long-term use and to target populations most likely to benefit from the intervention in order to improve safety.
The investigators’ specific goal was to assess the proportion of patients with RMDs thattransition to long-term opioid use after treatment initiation, looking at 6 RMD conditions and using 3 definitions of long-term use from the contemporary literature (Figure).
The team searched anonymized medical records of adults aged ≥18 years entered into the Clinical Practice Research Datalink, a nationally representative UK-wide primary care research database, for those with a diagnosis of rheumatoid arthritis, psoriatic arthritis (PsA), axial spondyloarthritis (AxSpA), systemic lupus erythematosus (SLE), osteoarthritis, and fibromyalgia and without prior cancer. Included were patients with a new episode of opioid use, (ie, no opioid prescriptions in the prior 2 years), prescribed up to 6 months before or any time after receiving 1 of the 6 diagnoses between January 1, 2006, and October 31, 2021. Inclusion required at least 1 full year of follow-up data, according to the study.
Figure
Jani and colleagues calculated the proportions of and the trends over time in long-term opioid use for each RMD as well as the overlap among the standard, stringent, and broad definitions of long-term use. The team tested trends using negative binomial regression models including year as a continuous variable.
FINDINGS
Investigators identified a total of 841 047 patients for inclusion in their analyses. The majority had a diagnosis of osteoarthritis (796 276) followed by fibromyalgia (21 189), rheumatoid arthritis (12 260), PsA (5195), SLE (3081), and AxSpa (3046).
The research team reported 1 081 216 new episodes of opioid use among the cohort. Of these, 16.8% of patients transitioned to long-term use using the standard definition, 11.1% using the stringent definition, and 21.9% using the broad definition. Jani and colleagues found that more than 97% of the opioid initiation episodes meeting any of the 3 definitions were captured by the broad criteria. Slightly less than half fulfilled all 3, they said.
Analysis of proportion of use revealed the highest proportion of long-term opioid users among the 6 disorders of interest were patients with fibromyalgia, followed by rheumatoid arthritis, and AxSpa (below).

In contrast, the lowest rate of long-term opioid use was observed among the cohort of patients with osteoarthritis, with rates of 16.4%, 10.7% and 21.4% using the standard, stringent, and broad definitions, respectively.
Results of their analysis of trends in opioid use over time found statistically significant increases in the proportion of patients with fibromyalgia who transitioned to long-term opioid, which rose from 21.7% to 33.0% between 2006 and 2019 and reached 28.9% in 2020. The researchers observed a statistically significant decreasing trend among those with rheumatoid arthritis, but the overall proportion in 2020 remained high at 24.4%.
The authors highlight that in previous work, 1 in 7, or 14.6% of patients initiating opioids for noncancer pain became long-term users of the analgesics. They stress that all patients with RMD had a higher rate of transition to long-term opioid use than the previous cohort, regardless of the definition applied.
“The findings warrant vigilance in practice of opioid prescribing for [rheumatoid and musculoskeletal conditions] since long term opioid therapy is associated with poor outcomes (eg, opioid dependence and opioid-related adverse events),” they wrote. Overall, they conclude, that the present work “provides a signal for further exploration.”
Reference: Huang YT, Jenkins DA, Peek N, Dixon WG, Jani M. High frequency of long-term opioid use among patients with rheumatic and musculoskeletal diseases initiating opioids for the first time. Ann Rheum Dis. Published online May 16, 2023. doi:10.1136/ard-2023-224118
Newsletter
Enhance your clinical practice with the Patient Care newsletter, offering the latest evidence-based guidelines, diagnostic insights, and treatment strategies for primary care physicians.