Image IQ: Recurrent Eyelid Purpura
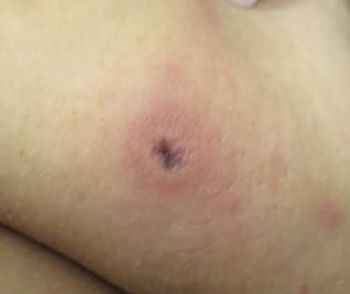
Eyelid bruising was observed on a 64-year-old woman during routine skin cancer follow-up. She denied trauma or pain. What does this look like to you?
A 64-year-old woman with a history of basal cell carcinoma presents to the dermatologist for skin cancer surveillance. She is incidentally noted to have bruising on her upper eyelids (above). On questioning, she reports experiencing recurrent intermittent eyelid bruising for several years. She denies a history of trauma to her face, pain, or other associated symptoms.
Her medical history is significant for hyperlipidemia, hepatitis C (diagnosed >30 years earlier), osteoporosis, celiac disease, and idiopathic proteinuria for several years. Her surgical history includes appendectomy and carpal tunnel repair.
Pertinent family history includes her mother dying of multiple myeloma and her father of complications of diabetes.
Review of systems is significant for vague symptoms of gastrointestinal discomfort. On more directed questioning, she reports the eyelid purpura is temporally related to the Valsalva maneuver/ strained bowel movements. Her medications include atorvastatin, risedronate sodium, a daily multivitamin, calcium, vitamin D, and aspirin.
Her examination reveals no bruising elsewhere and no findings of interest on skin or mucous membranes.
The patient is showing signs of:
Newsletter
Enhance your clinical practice with the Patient Care newsletter, offering the latest evidence-based guidelines, diagnostic insights, and treatment strategies for primary care physicians.
Related Content






























































































































