Lorundrostat Phase 2 Trial Results Suggest Potential Efficacy Against Uncontrolled and Resistant Hypertension
The selective aldosterone synthase inhibitor will move into late stage clinical trials, a nod to the potential for a first-in-class agent targeting aldosterone.
The investigational selective aldosterone synthase inhibitor lorundrostat was associated with clinically and statistically significant reductions in systolic blood pressure (BP) in persons with uncontrolled or resistant hypertension, according to results of a new phase 2 dose-finding study published in the Journal of the American Medical Association.1
Effects on systolic BP observed in the randomized placebo-controlled Target-HTN trial were particularly evident among participants with hypertension and concomitant obesity, according to study authors. Dosed at 12.5 mg twice daily and 50 and 100 mg once daily in the study, the safety profile of lorundrostat appeared favorable.
©dacasdo/stock.adobe.com

“Despite the multitude of currently available treatments, half of all patients treated for hypertension are not able to reach their blood pressure goal,” said Luke Laffin, MD, lead investigator and codirector of the Center for Blood Pressure Disorders in the Heart, Vascular, and Thoracic Institute at Cleveland Clinic, in a statement from biopharmaceutical company Mineralys Therapeutics.2 “Up to 25 percent of all people with hypertension exhibit abnormal aldosterone levels,” he continued.2 And yet current clinical guidelines recommend similar medication combinations for most patients, regardless of comorbidities or dominant underlying driver of hypertension, authors wrote.1 “Importantly, the Target-HTN study of lorundrostat demonstrated data compelling enough to warrant its advancement into late-stage clinical trials.”2
Further study of the first-in-class agent will advance understanding of treatment that targets the underlying causes of uncontrolled and treatment-resistant hypertension, Laffin added.
The prospective, multicenter phase 2 Target-HTN trial was conducted at 43 sites across the US and enrolled a population of adults aged ≥18 years, with a systolic automated office blood pressure (AOBP) measurement of ≥130 mm Hg while taking 2 or more antihypertensive medications for at least 4 weeks at maximum tolerated doses. Laffin and colleagues recruited participants into 2 cohorts, an initial group of 163 individuals with suppressed plasma renin (plasma renin activity [PRA] ≤1.0 ng/mL/h) and morning serum aldosterone of ≥1.0 ng/dL and a subsequent cohort of 37 participants with PRA of >1.0 ng/mL/h.1
Participants enrolled in cohort 1 were randomly assigned to receive placebo or lorundrostat at a dose of 12.5 mg, 50 mg, or 100 mg once daily or 12.5 mg or 25 mg twice daily. Those in cohort 2 received random assignment to placebo or lorundrostat 100 mg in a 1:6 ratio.
Investigators screened and enrolled participants between July 2021 and June 2022, with the final follow-up occurring in September 2022. Mean age among the full cohort of 200 was 65.7 years, 60% were women, 36% were Black or African American, and 48% were of Hispanic or Latino ethnicity.
Characteristics recorded at baseline for the full cohort1:
- 48% BMI <30 kg/m2
- 40% type 2 diabetes
- 42% treated with ≥3 antihypertensive medications
Mean baseline AOBP
- Cohort 1: mean systolic142.2 mm Hg, mean diastolic 81.5 mm Hg
- Cohort 2: mean systolic 139.1 mm Hg, mean diastolic 79.1 mm Hg
The primary endpoint of interest for the research team was change in AOBP from baseline to week 8. They identified secondary endpoints of interest as changes in diastolic AOBP, 24-hour ambulatory BP monitoring changes, and the proportion of participants achieving AOBP <130/80 mm Hg at week 7 or 8.1
FINDINGS1
Among participants in cohort 1 (PRA≤1.0 ng/mL/h) changes in systolic AOBP from baseline to week 8 were −14.1, −13.2, −6.9, and −4.1 mm Hg for groups receiving once-daily lorundrostat of 100 mg, 50 mg, and 12.5 mg and placebo, respectively.
Among those randomly assigned to twice-daily dosing, researchers reported reductions in systolic BP of −10.1 for the 25 mg group and −13.8 mm Hg for the 25 mg group.
Laffin et al found the least-squares mean difference between treatment with placebo and lorundrostat in systolic BP was −9.6 mm Hg (90% CI, −15.8 to −3.4 mm Hg; P = .01) for the 50-mg once-daily dose and −7.8 mm Hg (90% CI, −14.1 to −1.5 mm Hg; P = .04) for 100 mg daily dose.
In the second cohort (without suppressed PRA), treatment with 100 mg lorundrostat once daily reduced systolic BP by 11.4 mm Hg, a reduction the investigators characterized as similar to that seen among participants with suppressed plasma renin activity who received the same dose.
In their discussion of exploratory endpoints, the authors pointed in particular to the greater decrease in BP in response to lorundrostat among participants with obesity (see below).
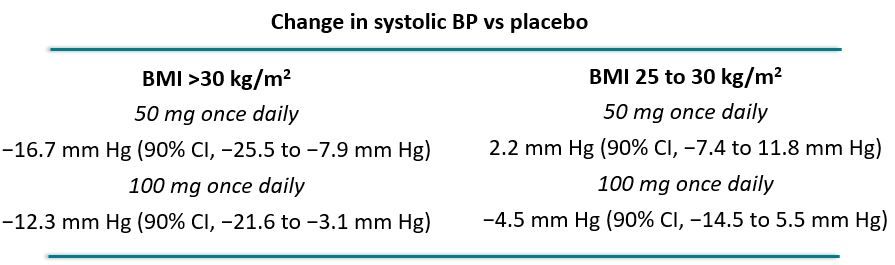
Safety and tolerability were favorable, the authors reported, with 6 participants experiencing increases in serum potassium >6.0 mmol/L, corrected with dose reduction or drug discontinuation. They reported no instances of cortisol insufficiency.1
In an editorial comment, Bryan Williams, MD, chair of Medicine at University College London, expressed excitement about the prospect of novel therapies addressing excess aldosterone.3
“More than 70 years after the first isolation of electrocortin, there is a new dawn for therapies targeting aldosterone,” Williams wrote.3 “There is now real potential to provide better-targeted treatment for patients in whom aldosterone excess is known to contribute to their clinical condition and influence their clinical outcome, notably those with difficult-to-control hypertension, obesity, heart failure, chronic kidney disease, and the many with yet-to-be-diagnosed primary aldosteronism.”