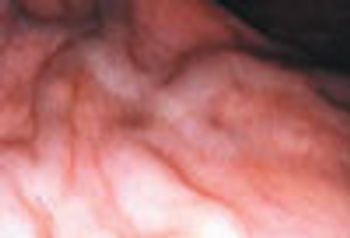
Loose, irregular bowel movements were the complaint of a 56-year-old man. He underwent colonoscopic examination. The dilated vascular structures shown are rectal varices: portosystemic collateral veins that develop with portal hypertension.

Loose, irregular bowel movements were the complaint of a 56-year-old man. He underwent colonoscopic examination. The dilated vascular structures shown are rectal varices: portosystemic collateral veins that develop with portal hypertension.

A 52-year-old woman presented to her primary care physician complaining of a nonproductive cough and dyspnea on exertion. These symptoms had a subacute onset over 4 weeks before her initial visit. She denied fever, sputum production, hemoptysis, chest pain, palpitations, abdominal pain, nausea, vomiting, and diarrhea. She did not have any known sick contacts.

A 53-year-old woman presented to the emergency department complaining of substernal chest pain that awoke her from sleep. The chest pain was associated with left shoulder numbness, radiating to her back, and was partially alleviated with sublingual nitroglycerin. During this episode, the patient had a cough productive of yellow phlegm and one instance of cough productive of 1 tbs of bright red blood.

A 52-year-old man presented to his primary care physician with shortness of breath for 5 days, right-sided lower thoracic back pain, and dry cough. The patient was a 15-pack-year cigarette smoker who had emigrated from China to the United States in 1989. He had no significant history of occupational exposure or tuberculosis. He had no significant weight loss, and his past medical history was otherwise unremarkable.

Abstract: In the assessment of central airway obstruction and disease, no imaging technique is an adequate substitute for bronchoscopy. The indications for rigid bronchoscopy include multiple malignant and benign disorders, with most interventions performed for treatment of complications of lung cancer. The rigid bronchoscope is a useful tool for managing most types of airway stenoses, and it facilitates other endobronchial therapies, including stent placement, argon plasma coagulation, balloon dilatation, electrocautery probes, and laser therapy. Certain patients with benign lesions or postintubation or post-tracheostomy stenosis may benefit from rigid bronchoscopic techniques instead of surgery. Although use of the rigid bronchoscope requires general anesthesia, it provides a stable airway and often results in fast removal of foreign bodies. (J Respir Dis. 2006;27(3):100-113)

Abstract: The manifestations of indoor mold-related disease (IMRD) include irritant effects, such as conjunctivitis and rhinitis; nonspecific respiratory complaints, such as cough and wheeze; hypersensitivity pneumonitis; allergic fungal sinusitis; and mycotoxicosis. The diagnosis of IMRD depends on eliciting an accurate history and excluding preexisting pathology that would account for the patient's symptoms. Laboratory tests, imaging studies, and spirometry can play an important role in ruling out other diagnoses, such as allergic or nonallergic rhinitis, asthma, and pneumonia. The diagnosis of IMRD also involves integrating the results of immunologic, physiologic, and imaging studies with the results of indoor air-quality studies. (J Respir Dis. 2005;26(12):520-525)

Abstract: Acute chest syndrome (ACS) is one of the most common causes of death and hospitalization among patients with a sickle hemoglobinopathy. The clinical presentation is characterized by the appearance of a new infiltrate on a chest radiograph, with 1 or more new symptoms, including fever, cough, chest pain, and dyspnea. Additional findings include leukocytosis, hypoxemia, and auscultatory signs of consolidation. The differential diagnosis includes pneumonia, pulmonary infarction, fat embolism syndrome, pulmonary edema, and bone infarction. Treatment of ACS involves supportive care, empiric antibiotic therapy, and red blood cell transfusion when indicated. The decision of whether to use simple or exchange transfusions depends on the severity of illness and the risk of acute respiratory failure. Currently, hydroxyurea is the only FDA-approved drug designated as a preventive therapy. (J Respir Dis. 2005;26(12):529-534)
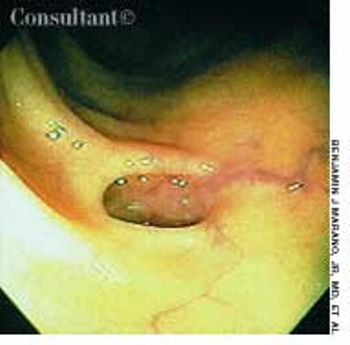
An 84-year old woman, who depends on a weekly dose of magnesium citrate to have a bowel movement, has extensive diverticulosis throughout the length of the colon.

Routine chest radiographs reveal a left lower lobe density in a 70-year-old man

Abstract: High-resolution CT (HRCT) can play an important role in the assessment of bronchiolitis. Direct signs of bronchiolitis include centrilobular nodules, bronchial wall thickening, and bronchiolectasis. Indirect signs include mosaic perfusion, hyperlucency, mosaic or diffuse airtrapping, vascular attenuation, and increased lung volumes. Expiratory HRCT scans are considered an essential part of the workup, because airtrapping may be evident only on these scans. In infectious cellular bronchiolitis, the centrilobular nodules typically have a branching, or "tree-in-bud," appearance, whereas in hypersensitivity pneumonitis, these nodules have a round or nonbranching pattern. The HRCT signs of constrictive bronchiolitis include mosaic perfusion, mosaic airtrapping, vascular attenuation, bronchiolectasis, and bronchiectasis; centrilobular nodules are usually absent. (J Respir Dis. 2005; 26(5):222-228)

March 1st 2006

May 1st 2005

December 1st 2005