Less than Half of Patients with New AF Diagnosis Prescribed Oral Anticoagulation within 6 Months
Among patients newly diagnosed with atrial fibrillation who were at high risk for stroke, less than half (41.3%) were prescribed oral anticoagulant (OAC) therapy within 6 months of that diagnosis, according to new research from investigators at the University of Colorado Medicine.
The odds of receiving a prescription for anticoagulation, as current clinical guidelines recommend for AF management, were associated with patient sex, race/ethnicity, and elevated CHA2DS2-VASc score, among other clinical factors, the authors found.
The research team, writing in the journal Clinical Cardiology, notes that OAC use is already known to be poor among eligible patients with AF and the authors cite regional and national data showing an overall prescription rate of approximately 60%.
“…increasing age and increasing HAS‐BLED scores,” are among patient factors known to be associated with reduced OAC prescribing, Evan Manning, MD, MPP, of the internal medicine residency training program at the University of Colorado (UC) Anschutz Medical Campus, Colorado, and colleagues wrote. Other studies have found negative associations between increasing Charlson Comorbidity Index scores and OAC prescribing.
There is less research, they say, on how clinical factors such as comorbidities and medications already on board may affect an initial OAC prescription. Current data come largely from studies that are geographically limited and were conducted before direct OAC (DOACs) were in widespread use.
For their study, the research team tapped data from an electronic health record (EHR) system shared by 11 community-based hospitals in the UC Health System network. Manning et al created a retrospective cohort comprised of 18 404 patients with a new diagnosis of AF between January 2013 and December 2018. Potential participants were excluded if they had an existing prescription for OAC, a CHA2DS2VASc score <2, were pregnant, or had valvular disease.
The outcome of primary interest was prescription of an OAC (vitamin K antagonist or DOAC) during the 6 months following an AF diagnosis. In secondary analyses, the investigators calculated the odds of an OAC prescription associated with 17 predefined clinical variables.
FINDINGS
The cohort of 18 804 individuals was approximately half men (53.0%) and had a median age of 73.9 years. Of them, 41.3% (7604) were prescribed an OAC within 6 months of an AF diagnosis with just more than one-third (35.8%) of those for DOACs.
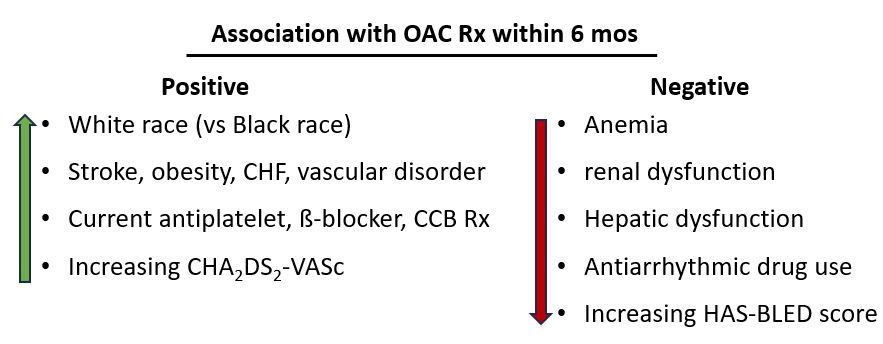
Of the 17 independent clinical factors evaluated, the following were positively associated with receiving an OAC prescription within the 6-month period: Male sex, white race (vs Black race), stroke, obesity, congestive HF, vascular disorders, current antiplatelet, beta-blocker, or calcium channel blocker prescription, and increasing CHA2DS2‐VASc score. Negatively associated with a timely OAC prescription were anemia, renal dysfunction, liver dysfunction, antiarrhythmic drug use and increasing HAS‐BLED score.
In their discussion, Manning et al wrote they would expect factors including bleeding risk, comorbid conditions associated with bleeding, and renal dysfunction to limit OAC prescribing. What they found “less intuitive” was the negative association between OAC use and antiarrhythmic drug (AAD) use, a result they hypothesize may be related to inclusion of patients with lower CHA2DS2‐VASc scores and paroxysmal AF, thus lower arrhythmia burden. Use of AADs also may signal a clinician’s “intent to pursue an antiarrhythmic strategy” and thus to forgo anticoagulation.
Either scenario, however, is “still contradictory to current guidelines in AF management,” they argue.
“The salient finding of this work,” they emphasize, “is less than half of those eligible for long‐term OAC with newly diagnosed AF receive timely therapy. As evidenced by our findings, patient‐level factors are associated with increased or decreased OAC prescriptions and may represent opportunities for targeted study and intervention to reduce the risk of stroke in the greater population. All these associated factors represent possible future directions of study.”
Reference: Manning E, Burns K, Laurie M, Patten L, Ho M, Sandhu A. Factors associated with oral anticoagulant prescription status among patients with a new diagnosis of atrial fibrillation. Clin Cardiol. Published online July 4, 2023. doi:10.1002/clc.24077 https://onlinelibrary.wiley.com/doi/full/10.1002/clc.24077
Newsletter
Enhance your clinical practice with the Patient Care newsletter, offering the latest evidence-based guidelines, diagnostic insights, and treatment strategies for primary care physicians.