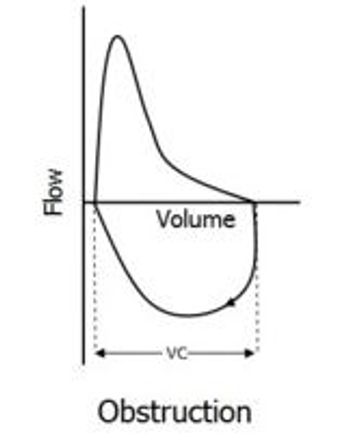
What do you get when you cross asthma with COPD? How does an asthma Dx reduce antibiotic Rx? And what about vitamin D and asthma, anyway? Get answers and evidence in 5 easy pages.

What do you get when you cross asthma with COPD? How does an asthma Dx reduce antibiotic Rx? And what about vitamin D and asthma, anyway? Get answers and evidence in 5 easy pages.

Recent studies have interesting implications for selecting medication and modifying asthma management. Clinician and researcher Barabara Yawn, MD, MSc provides a review-and offers insights on practical implications for primary care.

Sleep complaints are common in patients with chronic obstructive pulmonary disease (COPD). Many patients complain of morning tiredness, early awakenings, difficulty in falling asleep, restlessness, and daytime sleepiness. Functional status may eventually be impaired by the resulting chronic fatigue that is compounded by dyspnea.

abstract: Depression and anxiety are common comorbidities in patients with chronic obstructive pulmonary disease (COPD), and like COPD, they are often underrecognized. Both of these comorbidities can adversely affect the course of COPD. Anxiety, for example, is associated with more severe dyspnea, greater disability, and impaired functional status; it also is a significant predictor of hospitalizations for acute exacerbations of COPD. When evaluating depressive symptoms, it is important to rule out cognitive impairment, particularly in patients with severe COPD and hypoxemia. Treatment options include antidepressants and cognitive behavioral therapy. Participation in a pulmonary rehabilitation program also can help reduce anxiety and depressive symptoms in patients with COPD. (J Respir Dis. 2007;28(3):94-103)

ABSTRACT: Many patients with presumed mild intermittent asthma have unrecognized persistent symptoms; these can be elicited with specific questioning about coughing, wheezing, shortness of breath, chest tightness, nighttime awakenings, and exercise intolerance. Asthma severity may vary with the season. For asthmatic patients with predictable seasonal allergies, prescribe inhaled corticosteroids for a few weeks or months beginning 2 to 3 weeks before usual symptom onset. Successful long-term management requires identification and control of asthma triggers, such as cigarette smoke, house dust mites, cockroaches, molds, and animal dander. Removing triggers or minimizing the patient's exposure to them may allow improved asthma control with lower dosages of corticosteroids.
February 2nd 2012

April 1st 2007
November 11th 2011

August 1st 2003

September 15th 2011