
Monu Khanna, MD, discusses challenges in managing pain in patients with obesity, effective pharmacological and nonpharmacological therapies, and more.

CagriSema Phase 3 Update: Weight Loss of Nearly 16% Seen in REDEFINE 2 Trial

Investigational Ketogenic Diet Pill BL-001 Shows Significant Weight Loss in Phase 1 Trial

Monu Khanna, MD, discusses challenges in managing pain in patients with obesity, effective pharmacological and nonpharmacological therapies, and more.
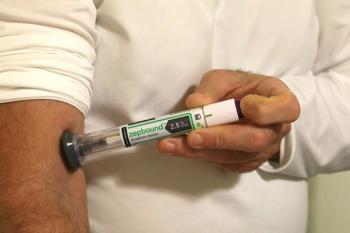
Eli Lilly launched 2 new strengths of Zepbound single-dose vials for self-pay patients, and lowered the price of 2.5 mg and 5 mg vials.

Shagun Bindlish, MD, discusses the complex interplay between obesity and mental health conditions and how sex is a potential moderating factor.

Anila Chadha, MD, highlights key preventive strategies to reduce CVD risk in patients with obesity and how to tailor them to address individual patient needs.

Merilog joins two long-acting insulin biosimilar products approved in 2021, bringing the total to three insulin biosimilars available in the United States.

Your daily dose of the clinical news you may have missed.
CELZ-201 reduced insulin dependency and stabilized HbA1c in 1-year follow-up data from a pilot study in T2D.

In letters to the FDA and Fox Broadcasting, PSM enumerated the laws abrogated and the potential harms of the ad being viewed by 200 million people on February 9, 2025.

Hardware or software changes as well as user adjustments may disable or mute alerts for elevated glycemia, medication use, and other diabetes management essentials, the agency said.

A GLP-1/GIP dual agonist in both subcutaneous and oral tablet formulations and a novel dual amylin and calcitonin receptor agonist lead the company's pipeline for antiobesity medications.

Premature menopause, authors said, should be included in diabetes management guidelines as a risk factor to support screening and prevention.

Anila Chadha, MD, talks to Patient Care about how antiobesity medications can aid in reducing CVD risk in patients with obesity.

An oral antibiotic for drug-resistant UTIs, a long-awaited therapy for congenital adrenal hyperplasia, and more.

In preliminary findings of the phase 2b QUALITY trial, 32% of weight loss in the semaglutide group was from lean mass reduction vs 9.4% in the combined semagutide/enobosarm group.

Weekly subcutaneous injections of amycretin featured a safety profile similar to other incretin-based drugs, according to new topline results.

Incretin-mimetics may have even broader application against disease than scientists can predict, but the risks are real, too, according to a study of 2 million.

The properties of ASC30 may allow the small molecule GLP-1 RA to be formulated as a monthly injection and daily oral tablet, Ascletis said.

Your daily dose of the clinical news you may have missed.
The 20.7% weight loss with the high-dose of semaglutide bested the mean reduction of 17.5% seen with semaglutide 2.4 mg, according to Novo Nordisk.

Your daily dose of the clinical news you may have missed.

"Glucocorticoid therapy in classic congenital adrenal hyperplasia: traditional and new treatment paradigms," offers an in-depth look at the disorder and promising therapies.

Shagun Bindlish, MD, board member of the American Diabetes Association, details available options for treating venous disease in patients with obesity.

More than half of study participants receiving the dual incretin agonist had weight loss of 20% or greater, with no evidence of a plateau and only mild AEs.
Atumelnant treatment resulted in statistically significant reductions in serum androstenedione and 17-OHP as well as notable improvements in CAH symptoms.

Elinzanetant produced a statistically significant reduction in frequency of treatment-related vasomotor symptoms as early as week 1 and in severity at weeks 4 and 12.