
Different strategies to prompt patients to take their antidepressant as prescribed have been tried. Many that have been evaluated in controlled trials are considered in a new review that examines their effectiveness.

Different strategies to prompt patients to take their antidepressant as prescribed have been tried. Many that have been evaluated in controlled trials are considered in a new review that examines their effectiveness.


The British medical journal, The Lancet, surveyed a number of studies that discuss troubling statistics on suicide and depression among American physicians.

Prenatal and Postpartum Depression Not Limited to Mothers
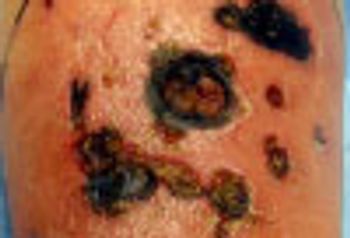
A 48-year-old African American man with no significant medical history sustained a gunshot wound to the face and shoulder.

Psychiatrist Sidney Zisook, MD-a guest speaker at the recent American College of Physicians meeting in San Diego

Twenty years ago, the American College of Rheumatology (ACR) introduced the following clinical criteria for the diagnosis of fibromyalgia (FM) . . .

Cannabis worsens cognitive function in patients with multiple sclerosis, reported investigators recently in the journal Neurology. Marijuana has been used to relieve the pain and spasticity associated with MS; however, the results of this study show that the drawbacks may outweigh the purported benefits

A variety of effective treatments are available for diabetic peripheral neuropathic pain (DPNP), including topical agents, oral medications, and nondrug approaches. The lidocaine patch 5% is recommended for relatively localized pain.

The treatment of chronic fatigue syndrome (CFS) is mainly supportive. The key to effective management is to establish a therapeutic alliance with patients and to convey a consistent message that their complaints are taken seriously. Although spontaneous recovery is rare, it does occur in some patients with CFS.
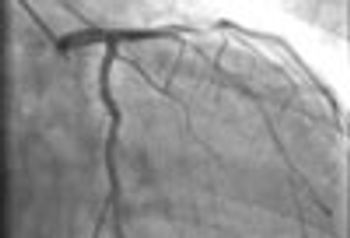
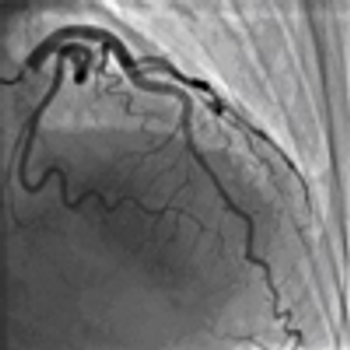
A 72-year-old obese man with chronic atrial fibrillation, hypertension, hyperlipidemia, and a history of tobacco use presented for a routine office visit. A year earlier, he began to experience recurrent chest pain, but an ECG had shown normal T waves.

Chronic fatigue syndrome (CFS) is a distinct disorder characterized by debilitating and often recurrent fatigue that lasts at least 6 months but more frequently lasts for longer periods. Patients with CFS experience overall physical, social, and mental impairments and may subsequently qualify for medical disability.
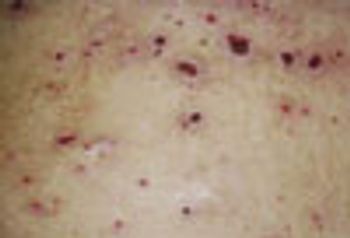
A 54-year-old woman presents for an initial consultation. She has multiple chronic disorders, including type 2 diabetes mellitus and hypertension, for which she takes various medications-none of which are new.

Primary care is demanding for a host of reasons, not the least of which is the daunting breadth of issues practitioners grapple with. One issue is evaluating the risk of suicide. Two recent studies provide some intriguing data that may change the way we practice.
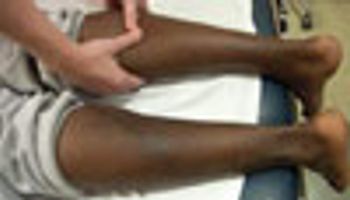
Does an Achille’s tendon rupture, tendonitis, bursitis, or something else underlie sudden heel and lower leg pain?

Quality of life in children and adolescents with inflammatory bowel disease (IBD) is a key focus of research presented at the 2010 Advances in IBD conference in Hollywood, Florida. Two of the top abstracts address social isolation and patient adherence to medication regimens among teenagers with IBD.

Diabetes is a demanding and difficult chronic disease. Life changes dramatically for a patient and his or her family once the diagnosis is made. Nutritional food choices, increased physical activity, multiple medications, visits to a physician, and blood tests are no longer optional. They now are a means of changing the length and quality of life. The patient has to rapidly become knowledgeable about nutritional content of any food he eats, different ways to be active, blood glucose testing, medication doses and side effects, and new words and abbreviations, such as A1c, LDL, HDL, and triglycerides.

How to determine whether opioids are appropriate, what to do about breakthrough pain, and how frequently to monitor.

Dr Schneider addresses myths and misunderstandings about the long-term use of opioids to treat noncancer pain.

According to the Sgarbossa criteria, the patient had an acute MI: ECG revealed a greater than 1-mm ST-segment depression in lead V2 and about 5-mm discordant ST-segment elevation in leads II, III, and aVF.

Selective serotonin reuptake inhibitors and other second-generation antidepressants have become common therapeutic options for the management of depression. Although these agents are effective and generally well tolerated, they frequently cause sexual adverse effects that can impact patients’ quality of life, thus ultimately leading to nonadherence to therapy in many cases.

Primary care physicians treat the majority of patients in this country who have mental health disorders. But how well prepared are we for these patients when they present to our offices?

In this podcast, Dr Lieberman discusses the associated features of three specific mental disorders: anxiety, major depressive disorder, and bipolar disorder. He offers practical techniques that can be used in diagnosing each of these disorders and provides suggestions for treatment.

Some women 75 and older who are in good health and have excellent functional status may benefit from mammography screening, while others who are in poor health and have short life expectancies probably do not.