
How can I control elevated blood pressure (BP) in an older patient who is already taking 4 antihypertensive agents?

How can I control elevated blood pressure (BP) in an older patient who is already taking 4 antihypertensive agents?

A tip to help motivate patients to make regular blood pressure checks.

BETHESDA, Md. -- A simple blood test for brain natriuretic peptide (BNP) has identified sickle cell patients with pulmonary hypertension, researchers here reported.

FRAMINGHAM, Mass. -- Children of parents who develop heart failure appear to be predisposed themselves to both left-ventricular systolic dysfunction and overt heart failure, researchers here reported.

BALTIMORE -- For an investigational beta-blocker found to have no beneficial effect on heart failure the story may not be over.

A 72-year-old man consulted his primary care physician because of confusion and vision loss of recent onset. He had no history of hypertension or diabetes.
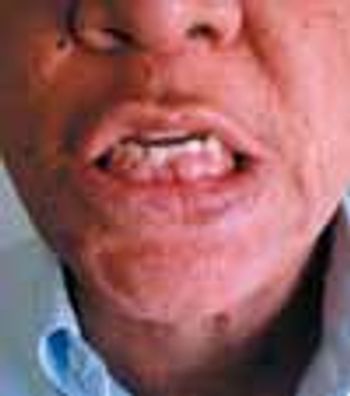
A 61-year-old man presented with swollen gums. His medical history was significant for hypertension. About 6 months earlier, he had started taking nifedipine, 60 mg/d. He was not taking any other medications.

UPPSALA, Sweden - A nighttime increase in diastolic blood pressure, or blood pressure that fails to dip at night, are significant independent predictors of congestive heart failure, researchers here reported.

ROCHESTER, Minn. - Patients with wide swings in blood pressure during the early hours of an ischemic stroke have a higher likelihood of death within three months, said researchers here.

The sale of simvastatin over-the-counter has been approved in the United Kingdom. Is this a first step in permitting other medications for asymptomatic diseases (such as hypertension) to be available over-the-counter? Dr Nash calls for a national debate on the availability of drugs to consumers.

WASHINGTON - For every five visits to primary care physicians by diabetic patients with blood pressure that's too high, only once will the antihypertensive regimen be intensified, according to researchers here.

Plumbing analogies can help asymptomaticpatients comprehend the seriousnessof elevated lipid and bloodpressure levels.

I have read that the concurrent use of an NSAID and an angiotensin-convertingenzyme (ACE) inhibitor may impair the antihypertensive effect of the ACEinhibitor. What is the mechanism of this interaction?

A 77-year-old woman who had hadanorexia and weakness for 3 monthswas seen after a syncopal episode. Sheappeared pale but alert. Heart rate was110 beats per minute; respiration rate,22 breaths per minute; and blood pressure,170/70 mm Hg. Her hematologicindices were: hemoglobin level, 4.3 g/dL;mean corpuscular volume (MCV), 60fL; mean corpuscular hemoglobin concentration(MCHC), 29 g/dL; red bloodcell count, 1.6 million/μL; white bloodcell count, 7500/μL; and platelet count,452,000/μL.

abstract: Pulmonary arterial hypertension (PAH) is a common complication in patients with systemic sclerosis and is associated with an increased mortality rate. Patients are often asymptomatic early in the disease, but as the disease progresses, exertional dyspnea and fatigue develop. The workup usually includes chest radiography, pulmonary function tests, and Doppler echocardiography. If the results of Doppler echocardiography are consistent with PAH, the patient should undergo right heart catheterization. Patients with mild PAH who demonstrate considerable vasoreactivity are potential candidates for treatment with oral calcium channel blockers. Other therapies that can reduce symptoms and improve exercise tolerance and hemodynamics include bosentan and epoprostenol.

According to previous reports, patients with pulmonary arterial hypertension (PAH) associated with collagen-vascular disease have a better prognosis than patients who have idiopathic PAH. However, in a study conducted in Korea, Chung and colleagues recently found that the mortality rate was significantly higher in patients with systemic lupus erythematosus and pulmonary hypertension (SLE-PH) than in those with idiopathic PAH.

abstract: Pulmonary hypertension is an increasingly recognized complication of HIV disease. Echocardiography is the most useful imaging modality for an early diagnosis; the most frequent findings are systolic flattening of the interventricular septum, right atrial and right ventricular enlargement, and tricuspid regurgitation. Other components of the workup include comprehensive laboratory tests (complete blood cell count, measurement of prothombin time and partial thromboplastin time, hepatic profile, etc), chest radiography, pulmonary function tests with arterial blood gas analysis, ventilation-perfusion lung scanning, and spiral CT scanning. The treatment of this condition is complex and controversial, and the drug of choice has not yet been established. The therapies currently used include antiretroviral agents, bosentan, calcium channel blockers, epoprostenol, and sildenafil.

Pulmonary arterial hypertension (PAH) can be difficult to diagnose because the symptoms are nonspecific and the physical findings are usually subtle (Table). In 2004, the American College of Chest Physicians (ACCP) published clinical practice guidelines for the diagnosis and management of PAH.1 Highlights of the ACCP's recommendations for patient assessment include the following:

The authors describe a woman who presented with severe pulmonary hypertension. A cardiopulmonary cause was initially sought, but thyrotoxicosis was the underlying cause.

abstract: Pulmonary arterial hypertension (PAH) is 1 of 5 types of pulmonary hypertension (PH). Symptoms may include dyspnea on exertion, fatigue, near-syncope, and palpitations. Physical findings include lower extremity edema, jugular venous distention, and a loud P2. Findings on chest radiography, transthoracic echocardiography, and electrocardiography can suggest the presence of PAH; however, right heart catheterization is the gold standard for confirming the diagnosis and for differentiating PAH from other forms of PH. It is essential to exclude chronic thromboembolic PH, since this can be surgically corrected. The treatment of PAH depends on the severity. In addition to the standard treatments, such as diuretics and anticoagulation, more advanced treatment options include prostaglandin therapy (epoprostenol, treprostinil, and iloprost), endothelin receptor antagonists (bosentan), and phosphodiesterase inhibitors (sildenafil).

A 53-year-old woman with a history of hypertension presents to the emergency department with excessive vaginal bleeding (requiring 6 or 7 sanitary pads per day), light-headedness, and episodes of near-syncope of 1 month's duration.

A 53-year-old man presents to the emergency department(ED) with chest pain that started the previous night. Thepain began about 30 minutes after he had smoked marijuanaand inhaled cocaine. He describes the pain as tightnessin the left side of the chest that radiates into theneck; he also has a tingling sensation in both the left sideof the neck and the left arm.

A 64-year-old woman with a history of uncorrected ventricular septal defect was hospitalized with progressive dyspnea and right heart failure. The patient had recently emigrated to the United States, where she received the diagnosis of ventricular septal defect with significant pulmonary arterial hypertension (Eisenmenger syndrome).

Abstract: Exercise intolerance is common in persons with chronic obstructive pulmonary disease and can result from multiple physiologic factors, including dynamic hyperinflation, gas exchange abnormalities, and pulmonary hypertension. In the initial assessment, keep in mind that many patients underestimate the degree of their impairment. The 6-minute walk test is very useful in assessing the degree of exercise intolerance; when more extensive assessment is indicated, cardiopulmonary exercise testing (CPET) is the gold standard. CPET is particularly useful for defining the underlying physiology of exercise limitation and may reveal other causes of dyspnea, such as myocardial ischemia or pulmonary hypertension. Strategies for improving exercise tolerance range from the use of bronchodilators and supplemental oxygen to participation in a pulmonary rehabilitation program. (J Respir Dis. 2006;27(5):208-218)

What factors are causing the increased incidence of hypertension and cardiovascular mortality in African Americans, and what can be done to counteract them?