
A 47-year-old man sees you for a check-up. He complains only of low energy and attributes it to recent weight gain. But, there is much more.

A 47-year-old man sees you for a check-up. He complains only of low energy and attributes it to recent weight gain. But, there is much more.

Unfortunately, the growing epidemics of hypertension and gout are often a package deal. Recent data demonstrate that 74% of people with gout are also hypertensive.
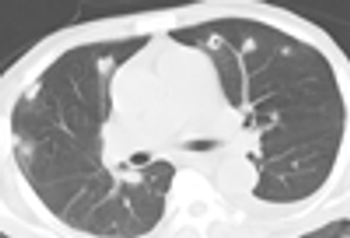

Dizzy patient? Their brain might not be getting enough blood, thanks to their antihypertensive dosage.


During my residency in medicine, and for a generation after, ß-blockers were among first choices for lowering blood pressure. Now it seems that ß-blockers have evolved into disreputable antihypertensives. What’s changed over a generation?
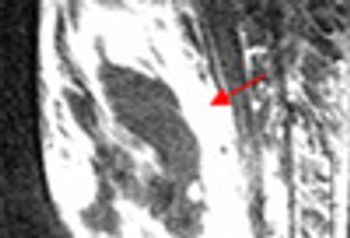
A 50-year-old African American woman with type 2 diabetes mellitus and hypertension was admitted with constant bilateral knee and thigh pain and swelling of both knees, all of 1 week’s duration. The pain was not relieved with hydrocodone/acetaminophen and had caused weakness and subsequent falls.

Prevalence for overweight (BMI 24.9 to 29.9) and obesity (BMI > 30) have been steadily rising for the past 30 years-two-thirds of Americans now qualify as overweight or heavier. Hypertension, hyperlipidemia, coronary artery disease, type 2 diabetes, sleep apnea, and GERD prevalence are following this epidemic. Obesity is now the second most common preventable cause of death, exceeded only by smoking.

Gout, once considered a disease of kings, is now a common and equal opportunity disease that affects as many as 3 million people in the US. Gouty arthritis has now become a serious problem in organ transplant recipients; in diuretic users; and in patients with CKD, hypertension, metabolic syndrome, heart failure, plus more.
The authors’ opening salvo seems to say it all (again). . . “A patient’s nocturnal BP profile, without the pressor effect of physical activity, emotional stress, and environmental factors that are usually present during the day, is more representative of the true BP status and a stronger predictor of cardiovascular outcomes.”

Typically, antihypertensive medications are taken in the morning. But typically does not always equal correct! Preliminary studies have documented that a more appropriate approach would be to take them (or at least some of them) at bedtime.

It should come as no surprise. The combination of the obesity epidemic and delayed childbearing in the US has fostered a novel mini-epidemic. Chronically hypertensive women are becoming pregnant in greater numbers. The trend is not just a perinatal and obstetric problem.

The era of controlling blood pressure with monotherapy (ie, with only a single antihypertensive) may well be a thing of the past. A recent American Society of Hypertension position paper on combination therapy in hypertension summarized the following pertinent observations in this regard.

A recent commentary of mine regarding hypertension was entitled, “Are Prescribing Practices for Antihypertensives Primitive? The Truth Hurts."
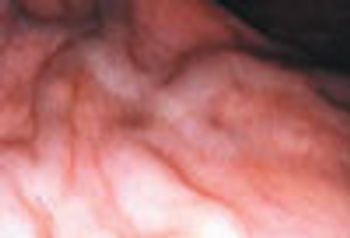
Loose, irregular bowel movements were the complaint of a 56-year-old man. He underwent colonoscopic examination. The dilated vascular structures shown are rectal varices: portosystemic collateral veins that develop with portal hypertension.

Measurement of pulse pressure may help identify patients with "white coat" hypertension, according to data presented by Korean researchers at the American College of Cardiology’s 60th Annual Scientific Session.

A panel of experts presented a general strategy for evaluating patients with refractory hypertension, but ultimately cautioned the audience to assume non-compliance until proven otherwise.

Diastolic heart failure (or HFPEF-heart failure with preserved ejection fraction) is characterized by inadequate myocardial relaxation and diastolic filling ("stiff ventricle"), with heart failure signs and symptoms despite normal ejection fraction. The most common cause is long-standing hypertension.

Researchers from Massachusetts General Hospital in Boston presented results from the PROTECT (ProBNP Outpatient Tailored Chronic Heart Failure) study. NT-proBNP (b-type natriuretic peptide) is a biomarker released from myocardial tissue in response to high levels of wall stretch and has been studied as a marker for decompensated systolic heart failure.
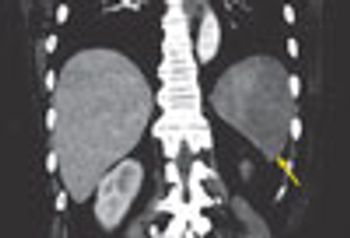
A 53-year-old woman presented with sudden onset of left upper quadrant abdominal pain. She had a history of atrial fibrillation, hypertension, and congestive heart failure.

On December 18, 2005, Ariel Sharon, Prime Minister of Israel, experienced the sudden onset of aphasia. Despite being overweight, he had none of the traditional risk factors for cerebrovascular disease-hypertension, history of smoking, diabetes, or elevated cholesterol levels.
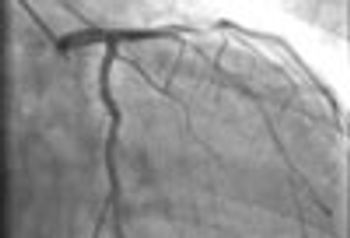
A 72-year-old obese man with chronic atrial fibrillation, hypertension, hyperlipidemia, and a history of tobacco use presented for a routine office visit. A year earlier, he began to experience recurrent chest pain, but an ECG had shown normal T waves.
The physical exam – looking into the eyes and throat, taking the blood pressure, sounding the chest – is part of the process of medical diagnosis. It's one way a physician attempts to determine the cause of a patient's complaint.
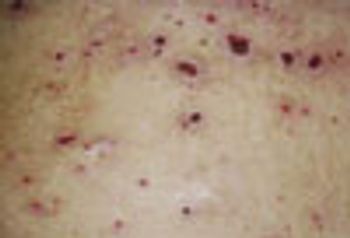
A 54-year-old woman presents for an initial consultation. She has multiple chronic disorders, including type 2 diabetes mellitus and hypertension, for which she takes various medications-none of which are new.