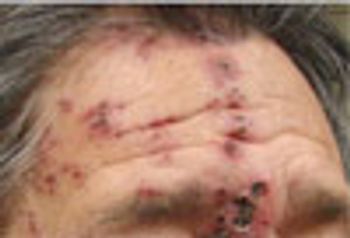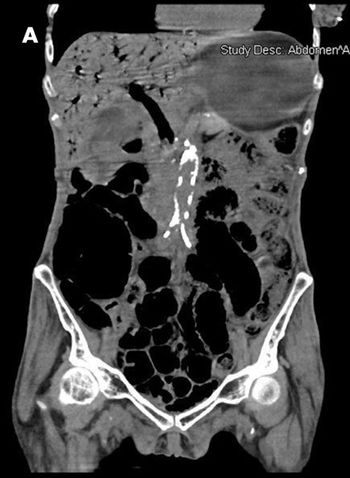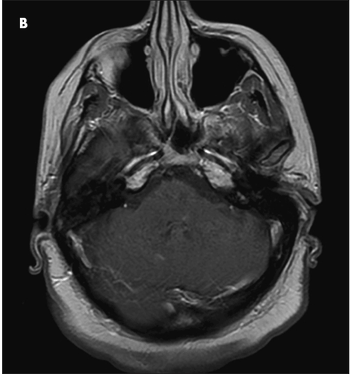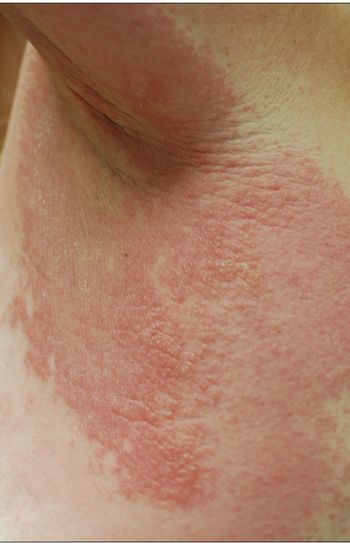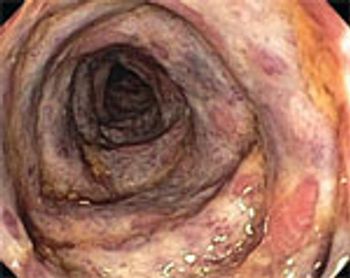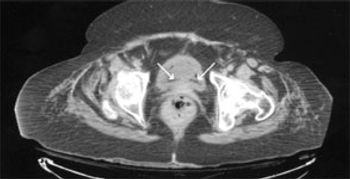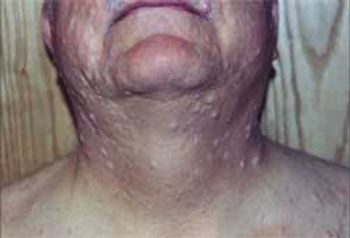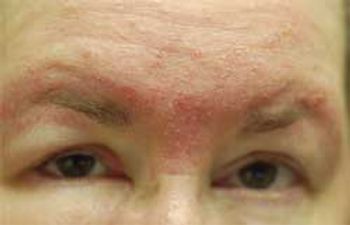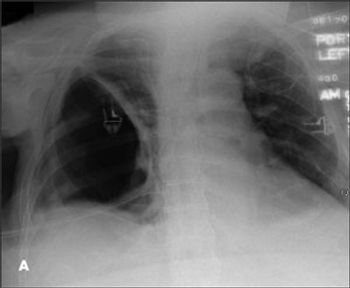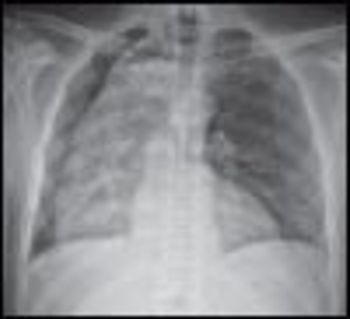
For the past year, a 52-year-old man had dysphagia, which he described as a “knot stuck in the throat” and an associated 25-lb weight loss. He denied fever, chills, headache, abdominal pain, and diarrhea. The patient had been living in the Dominican Republic until about 1 year earlier, when he moved to the United States. He had a 30 pack-year smoking history; he also had hypertension, asthma, and coronary artery disease (none of which were pharmacologically treated). He denied alcohol and illicit drug use.